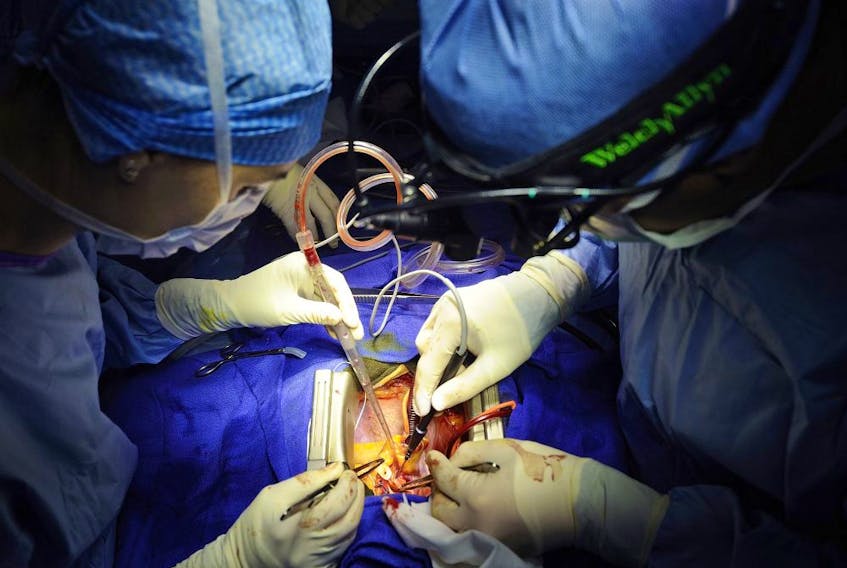
Vancouver surgeon Dr. Brian Day launched a challenge of the British Columbia Medicare Protection Act (MPA) in 2009, claiming that two Charter rights were violated, including a patient’s right to timely care.
The matter went to the B.C. Supreme Court in 2016, and final testimony was given on Feb. 28, 2020 – well before the global impact of COVID-19 was appreciated in Canada and the United States.
Justice John J. Steeves dismissed the court challenge in a report released on Sept. 10, 2020. He upheld three provisions of the MPA, including bans on extra billing, selling insurance for “medically necessary care” and permitting doctors to practise simultaneously in the public and private systems. However, he did acknowledge that, “some of these patients will experience prolonging and exacerbation of pain and diminished functionality as well as increased risk of gaining full benefit from surgery.”
In British Columbia, over the three years prior to the pandemic, over 18,000 elective surgeries had been added per year. When surgeries were cancelled or postponed due to COVID-19, everything changed. By early May, some 93,000 persons were on a wait list for surgery. Over just two months, about 30,000 operations had been cancelled or postponed. Two years and $250 million would be required to work through this.
One model predicts that across Canada, wait times may increase by a factor of four to seven due to COVID-19. Even prior to the pandemic, 308 patients per year in the B.C. Fraser health region died annually on wait lists — or 18 per day in Canada.
Legalizing some private care would not necessarily deplete the public system of surgeons. For years, according to the Royal College of Physicians and Surgeons of Canada, there has been a fundamental problem with workforce planning in health care; underemployment in certain specialties has been worse since this problem began to be studied in 2011.
Some 19 per cent of specialists who passed certification exams in 2017 could not find a job right away. This especially affected those in neurosurgery, radiation oncology and orthopedic surgery. It was largely due to a lack of funding for operating room time, recovery beds, and nursing support.
In 2018, the Canadian Orthopaedic Association reported that of 478 residents who completed their training over the previous six years, 159 were still seeking full-time employment and 74 were working full-time outside of Canada.
In addition, nearly 4,300 Canadian nurses work in the U.S. When polled, half indicated this was because they had been unable to find full-time work in Canada.
Prior to the pandemic, there was always the “safety valve” of travel outside of Canada for those who were unwilling to wait.
Those from the Atlantic provinces might seek care in Boston, New Haven, New York — or other countries.
According to the March 2019 policy brief by Second Street entitled “Flight of the Sick,” in 2017, some 217,500 Canadians sought health care in the United States and several other countries, and spent $690 million. In addition, their accompanying relatives spent money on hotels, restaurants, shops, etc., and stimulated the local economy.
However, because of the current high prevalence of COVID-19 in many of these regions, most Canadians will be deterred from leaving their own country.
One option does remain: the Canada Health Act does not apply when one obtains private health care in a different province. Many private clinics exist in Quebec. For example, many Ottawa patients pay about $800 for an MRI scan to be done in 24-48 hours across the river in Gatineau, Que. Also, a private surgical facility in Laval (near Montreal) will perform a total knee or hip replacement for $22,000 with a wait time of five to six weeks. The CHA restrictions also do not apply for certain groups — i.e., federal prisoners, professional athletes or WSIB patients.
The testimony in British Columbia failed to anticipate the severity of COVID-19. Not only has it greatly prolonged wait times in the public system, but Ottawa and the provinces have become deeply indebted, and can hardly afford the funds for needed augmentation of elective surgery operating room time, much less pay for the increased number of physicians, nurses and other health professionals.
Canada is the only country in the world that outlaws private insurance and care for most of its residents. In 2017, the Commonwealth Fund concluded that Canada ranked ninth out of 11 high-income countries in health-care delivery; those at the top had a mixed private/public system.
Because of COVID-19 or any future pandemics, patients in Canada now lack the ability to easily seek more timely surgical care or investigations in the United States or other countries.
Should there not be a private option available to them for treatment in their home province, even if they are not a member of one of these special groups? This would likely shorten wait times and provide employment in Canada for many MDs and nurses who might otherwise leave for other countries. It would put millions of dollars back into the Canadian economy at a time when it is sorely needed.
Ottawa physician Dr. Charles S. Shaver is past chair of the section on general internal medicine of the Ontario Medical Association. The views expressed here are his own.