CHARLOTTETOWN, P.E.I. — One man is dead after an accidental opioid overdose on Friday, said Dr. Heather Morrison.
She announced the death at a scheduled media briefing on COVID-19 Tuesday.
Friday’s victim, a male in his 40s, is the third death in this province due to an accidental overdose involving fentanyl this year.
In May a woman in her 20s died, then in July, a male in his 20s died. In both cases, they were accidental mixed-drug deaths involving fentanyl.
P.E.I. has counted two deaths – one in 2016 and one in 2018 – since the province began tracking accidental opioid-related deaths in 2016.
Not all opioid overdoses are fatal, she said. Most overdoses are mixed-toxicology, meaning they involve one or more opiates and one or more non-opiate substances, such as alcohol, said Morrison.
Good to know
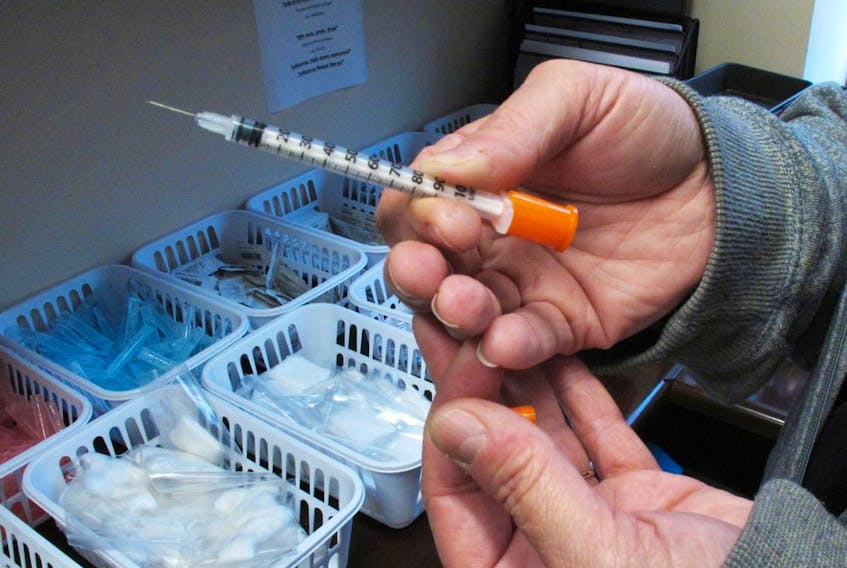
The Needle Exchange Program is available across the province to prevent the transmission of hepatitis B, hepatitis C and human immunodeficiency virus (HIV) spread by sharing equipment to inject drugs.
The program is a harm reduction initiative and offers services such as:
- Needle exchange with safe needle disposal
- Immunization counseling and immunization
- Vein/wound care
- Sexual health counseling
- Health teaching to support optimal health
- Referrals to other care providers
- Naloxone kits for people who are at risk of opioid related overdoses
Clinics:
Charlottetown - Boardwalk Professional Centre, 220 Water St.
Montague - Public Health Nursing, 126 Douses Rd.
Souris - Public Health Nursing, Lower Level, Souris Hospital
Summerside - Harbourside Medical Centre, 243 Heather Moyse Dr.
O'Leary - Community Hospital, 15 MacKinnon Dr.
Alberton - Western Hospital, 148 Poplar St.
Tignish - Tignish Medical Centre, 248 Philip St.
Call Public Health Nursing to confirm locations and clinic times: 1-877-637-0333
From January to March 2020 there were no overdose cases. From April to June, there were nine opiate-related overdoses that were not fatal; six involved fentanyl. From July to September, at least three overdoses involved fentanyl, but they were not fatal.
“Anyone consuming street drugs, not only opiates, but any drug in pill or powdered form, should take steps to reduce the risks. Carry naloxone and inform others who may use drugs that naloxone is available.”
Also part of the surveillance, a Narcan-alert system flags each time Island EMS administers Narcan. Additionally, Morrison sent a letter to all doctors and nurse practitioners asking that they test for opiates in all overdose situations. She has also met with the coroner, police and public health officials to discuss a rapid response to opiate related overdoses.
“It’s a variety of approaches that we need, not just to continue, but also augment, as we look at what’s happening here and also around the country. They’ve seen this situation in other parts of the country, and it’s of grave concern. We need to continue to do more, so I think you’ll see more about overdoses and what we can do to continue to educate everyone,” she said.
Morrison urged anyone consuming street drugs in pill or powder form to be careful and to have a naloxone kit nearby.
Kits are available through the provincial needle-exchange program. To confirm clinic locations and times, call 1-877-637-0333.