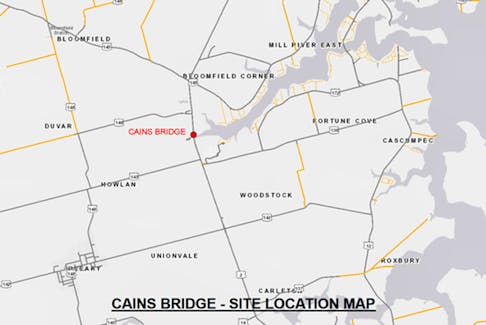
Top stories in Prince Edward Island
Local
MoreOpinion
MoreBusiness
MoreLifestyles
MoreSports
MoreCanada
MoreWorld
MoreHuge blast at military base used by Iraqi Popular Mobilization Forces, army sources say
BAGHDAD (Reuters) - A huge blast rocked a military base used by Iraq's Popular Mobilization Forces (PMF) to the south of Baghdad late on Friday, army sources told Reuters. (Reporting by Ahmed Rasheed; Editing by Chris Reese)
Updated 13 minutes ago
|1 min read